Discovery of a new drug target could lead to novel treatment for severe autism
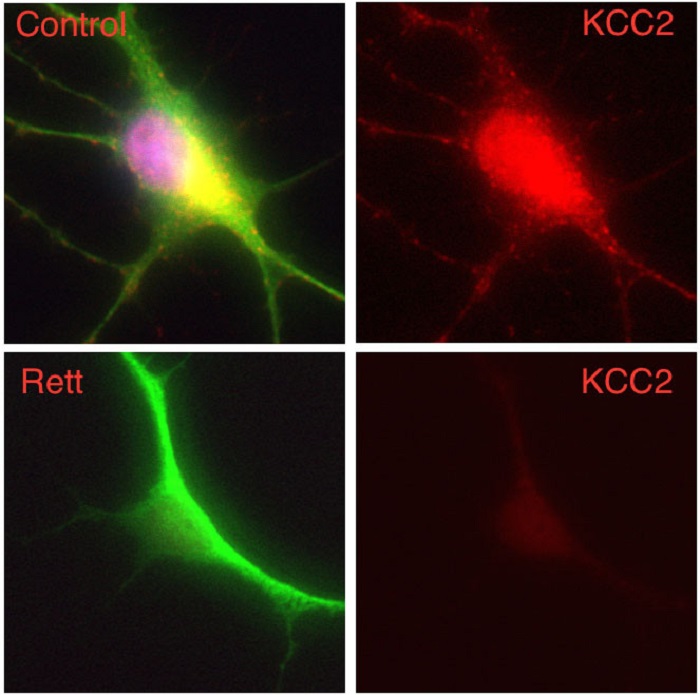
Photo Credit: Gong Chen lab, Penn State University
A novel drug target has been used to rescue functional deficits in human nerve cells derived from patients with Rett syndrome, a severe form of autism-spectrum disorder. The research could lead to a new treatment for Rett syndrome and other forms of autism-spectrum disorders, say investigators.
Anxiety genetics from chickens to humans

Photo Credit: Linköping Universitet
Mood-based disorders are one of the top-ten causes of disability worldwide. However the genes underpinning these disorders have proven to be remarkably elusive, say investigators. This study demonstrates that chickens are an excellent model organism for the genetic dissection of behavior.
Intriguing gender differences found in autistic friendships

Photo credit: hepingting via Foter / CC BY-SA
Could gender differences in the symptoms of autism mask their prevalence in girls? A recent study into autistic friendships highlights some striking asymmetries. According to Sedgewick: "Autism is seen as being much more common in boys because more boys than girls are diagnosed as being on the spectrum. This may be because diagnostic tools and criteria have been developed with boys and so are more biased towards identifying a 'male presentation' of autism.
Shared and Distinct Defects in ASD and Schizophrenia found in mice

Photo credit: hepingting via Foter / CC BY-SA
An article published in the Neuron Journal about Mice with Shank3 Mutations Associated with ASD and Schizophrenia Display Both Shared and Distinct Defects highlighting (1) Major psychiatric disorders share many risk genes; (2) Two mouse lines with ASD-linked and schizophrenia-linked mutations were studied; (3) Two mutant lines show both shared and distinct synaptic and behavioral phenotypes, and (4) Both developmental and molecular differences were detected in the two mutant lines